Doctor’s Notes
from Three Lamps Medical Centre, Auckland New Zealand
Medical practice changes over time and these notes, which date from many years ago, are provided for historical interest. They should not be used as a guide to current clinical practice.
Contents
Activated charcoal—substances for which its use is not indicated
Allergic rhinitis—treatment by desensitisation
Anal fissure—treatment with GTN
Ankle and foot xray, indications for
Australian RNA arbovirus infections causing polyarthritis
Asthma—betamethasone stat dose
Baldness, male-pattern. Hamilton-Norwood rating scale image
Baldness, male-pattern. Use of minoxidil and finasteride
Barmah Forest Virus and Ross River Fever (Australian RNA arboviruses)
Berger’s IgA nephropathy
Betamethasone. Stat dose in asthma
Brief dementia screening tool—Mini-Mental State Examination
Bupropion in smoking withdrawal
Calcium oxalate renal stones—dietary prevention of recurrence
Cataract—types
Cholecalciferol (vitamin D3) levels
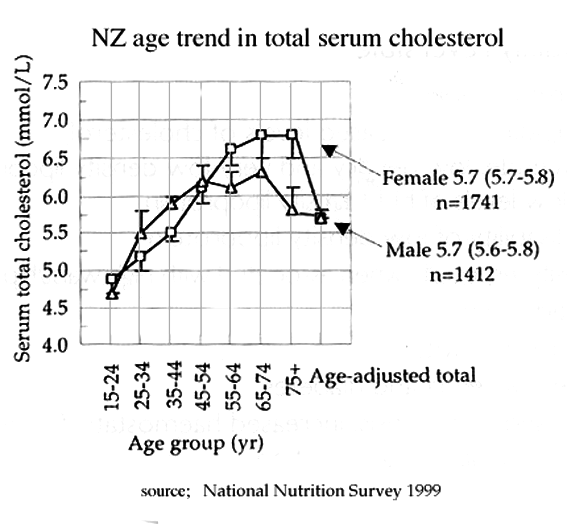
Cholesterol; total serum cholesterol by age in NZ
Chronic fatigue syndrome—differential diagnosis
Colic and reflux in infants and notes on feeding
Congenital HCV infection
Cracked teeth, prevention of
Croup—use of dexamethasone
Cystic fibrosis mutation testing
Deep Vein Thrombosis in the ‘Economy Class Syndrome’
Dental pain, unexplained
Depression. Use of Hypericum perforatum (St John’s wort)
Desensitisation for allergic rhinitis
‘Detoxification’ (withdrawal after methadone use)
Dexamethasone for croup
Diabetes—laboratory values for diagnosis
Diabetes, sugar and the glycemic index
Dietary stablising factors for warfarin use
Diabetes—use of nocturnal insulin supplementation of oral agents in NIDDM
Disease Modifying Anti-Rheumatic Drugs (DMARDs) in rheumatoid arthritis
Drug dosage in children (Salisbury approximation)
Dry mouth—use of pilocarpine
Dry skin—care of
‘Economy Class Syndrome’ and deep vein thrombosis
Ectopic pregnancy
Emergency Contraceptive Pill (‘Morning-after pill’)
Emollient action by formulation
Endocarditis prophylaxis with antibiotics before dentistry
Etidronate (Didronel) for osteoporosis
Eye, acute disorders of the
Eye examination in infants
Finasteride and minoxidil in male-pattern baldness
Fine needle aspiration
Folic acid in gastroenteritis
Fractures and dislocations of the nose
Gastroenteritis—use of folic acid
Genetic testing for hemochromatosis
Glucosamine for osteoarthritis
Glucose and HbA1c, correlation of levels
Glycemic index, diabetes and sugar
Glycerol trinitrate for treatment of anal fissures
Gonorrhea, current treatment in NZ (2004)
Hamilton-Norwood rating scale for male-pattern baldness
HbA1c and glucose, correlation of levels
Helicobacter pylori—triple therapy
Hemochromatosis and genetic testing
Hemolytic jaundice
Hepatitis C Virus infection—vertical transmission
Hepatocellular jaundice
Herpes Simplex Virus serology
Hip disorders in children by age of onset
HSV serology
Hypericum perforatum (St John’s wort); use in depression
Hypermetropia, testing for, with +2D glasses
Imiquimod. Use for ablation of skin lesions
Infant feeding in relation to colic and reflux
Infertility
Itraconazole—oral use in mycoses
Jamieson, K, on Living with Lithium
Jaundice, types of
‘Jet-lag’. Use of melatonin
Keratolysis, pitted
Kidney function and nephrotoxic agents
Laboratory values for diagnosis of diabetes
Leptospirosis
Lithium, living with (Kay Jamieson)
Malaria; treatment of P. vivax
Medroxyprogesterone acetate (depo-provera IM)—management of bleeding
Meningococcal septicemia or meningitis, emergency treatment
Melatonin as a hypnotic and for jet lag
Methadone—inpatient withdrawal
Mini-Mental State Examination—a brief dementia screening tool
Minoxidil and finasteride in male-pattern baldness
‘Morning-after pill’ (Emergency Contraceptive Pill)
Mycoses. Use of oral itraconazole
Myocardial infarction; diagnostic use of cardiac troponin
Nasal fractures and dislocations
Neisseria Meningitidis, emergency treatment
Nephropathy, Berger’s IgA type
Nephrotoxic agents
Nocturnal insulin supplementation of oral agents in NIDDM
Nomenclature
Obstructive jaundice
Ophthamological examination in infants
Opthalmology—common acute problems
Orlistat, a new drug for obesity
Orthopedic guidelines, acute presentations
‘Ottawa rules’ for ankle and foot xrays
Osteoarthritis—use of glucosamine
Osteoporosis—use of etidronate
Pediatric disorders of the hip by age of onset
Pediatric drug dosage calculation (Salisbury method)
Pediatric eye examination
Pilocarpine for xerostomia
Pitted keratolysis
Plantar warts, topical treatment
Plasmodium vivax malaria
Polycystic kidney disease
Pot sizes
Pregnancy, ectopic
Prophylaxis against endocarditis with antibiotics before dentistry etc
Pruritis, symptomatic treatment
Reflux and colic in infants and notes on feeding
Renal function and nephrotoxic agents
Retinal blindness; thromboembolic causes
Ross River Fever and Barmah Forest Virus (chronic Australian RNA arboviruses)
Rheumatoid arthritis—Disease Modifying Anti-Rheumatic Drugs (DMARDs)
Salisbury approximation for pediatric dosage
Serology of Herpes Simplex Virus
Serotonin syndrome, the
Skin, care of dry
Skin lesions, ablation of with imiquimod
Smoking cessation
Snoring, treatment by radio frequency tissue volume reduction
Stones, renal—dietary prevention of recurrence
Technique of fine needle aspiration
Teeth, prevention of cracking
Temperature, tympanic, normal range
Test for hypermetropia using +2 diopter glasses
Tooth, painful, unexplained
Thromboembolic causes of retinal blindness
‘Triple therapy’ for Helicobacter pylori
Troponin, diagnostic use in myocardial infarction
Tympanic temperature measurement norms
Vaginal bleeding after first dose of medroxyprogesterone acetate
Vertical transmission of Hepatitis C Virus infection
Vitamin D3 levels
Warts, topical applications
Xerostomia—use of pilocarpine solution and other measures
Xrays of ankle and foot after injury (Ottawa rules)
Activated charcoal—substances for which its use is not indicated
DdeC 12 February 1997
Simple ions (eg lithium, iron, cyanide)
Strong acids and alkalis
Alcohols (eg ethylene glycol, ethanol, methanol)
Dose of activated charcoal: 1–2 mg/kg oral or by nasogastric tube
source: Aickin, New Ethicals Feb 1977 p 34
Anal fissures, treatment with GTN
DdeC 24 February 1997
for chronic anal fissure, application of 0.2% glyceryl trinitrate ointment in soft paraffin twice daily (GTN ointment available as 2%)
source: Lund et al Lancet 349:11 1997 as reported in MedAlert 19/297
Ankle and foot xrays, indications for (Ottawa rules)
Indications for xray of ankle or foot after trauma, according to the “Ottawa Rules”
DdeC 6 October 2002
Xray of ankle is indicated if…
there is pain in the malleolar zone after injury
and
- tenderness at the tip of the lateral or medial malleolus or of the posterior aspect of the fibular or tibia for 6cm proximally
or
- inability to weight bear both immediately after injury and during examination (four steps, regardless of limping)
Xray of foot is indicated if…
there is pain in mid-foot after injury
and
- tenderness at the base of the 5th metatarsal laterally
or
- tenderness of the navicular bone medially
or
- inability to weight bear both immediately after injury and during examination (four steps, regardless of limping)
source; Premec Case Studies, September 2002
Barmah Forest Virus and Ross River Fever (Australian arbovirus infections causing ‘endemic polyarthritis’)
Two nonfatal Australian RNA arboviruses with acute symptoms at onset and chronic polyarthritic sequelae.
DdeC 6 March 2003
Barmah forest virus (named after a swampy forest on the Murray River near Echuca in northern Victoria)
- area: eastern states of Australia
- transmission: mosquito bites. Passed on by asymptomatic human carriers [?]
- periodicity: peaks in late summer at time of mosquito activity
- affected: males>females, elderly
- presentation: septicemia
- symptoms: migratory arthralgias, myalgia, intermittent fever, headache, may be rash
- diagnosis: serological test available
- treatment: nonspecific; rest, NSAIDs
- natural history: settles over months without specific treatment but may recur.
Ross River fever (named after a river at Townsville in north Queensland)
- area: northern Australia, Riverina irrigation area in NSW, New Guinea, Solomon Islands, Samoa, Fiji
- transmission: by mosquito bites. Carried by humans and probably bats.
- periodicity: peaks in late summer at time of mosquito activity
- affected: symptoms worsen with age. Children may be asymptomatic reservoirs of infection.
- presentation: epidemic polyarthritis
- symptoms: fevers, myalgia, peripheral arthritis, joint swelling, headache, adenitis, anorexia, nausea, fatigue, may be rash
- diagnosis: serological test available
- treatment: nonspecific. NSAIDs, antipyretics
- natural history: may be debilitating for months and may recur.
source; Warwick Carter (Brisbane) NZGP March 2003 p. 9
note; ‘arbovirus’ is a non-taxonomic term for viruses borne by arthropod vectors (Wikipedia)
Berger’s IgA nephropathy
DdeC 27 April 1998
A relatively benign condition causing recurrent macroscopic hematuria in childhood,
Case: recurrent macroscopic hematuria sometimes with assd. low abdo pain in 8yr old Polynesian girl.
History of penicillin courses after throat swabs positive for strep.
Bp 100/60 at 50 kg.
Bergers is mostly benign, not associated with hypertension, uremia, hypocomplimentemia.
Check for these and strep titres.
source: Ralph Pinnock pediatrician ACH
Betamethasone, stat dose in asthma
DdeC 24 November 1997
Recommended stat (or daily for 2–3 days) dose of betamethasone sodium sodium phosphate (‘Betnesol’) is 0.3 mg/kg up to up to 6 mg.
This is 12 tablets of 0.5 mg. At 6 x potency of prednisone equivalent to about 36 mg prednisone.
The dosage is based on a dose of 2 mg/kg prednisone
One year old child is about 10 kg (-> 3 mg Betnesol)
Five year old child is about 18 kg (-> 5.5 mg Betnesol)
(Ten year old child is about 30 kg)
See cautions in Bernadette Salmon’s article New Ethicals Sept. 1992 p 45
Half life of betamethasone is long.
from conversation, Onehunga A & E Clinic, 23/11/97
Brief dementia screening tool—Mini-Mental State Examination (MMSE)
DdeC/ED 14 March 2000
| question | points |
|---|---|
| 1. What day of the week is it? | 1 |
| 2. What is the date today? | 1 |
| 3. What is the month? | 1 |
| 4. What is the season? | 1 |
| 5. What is the year? | 1 |
| 6. Where are we now? | 1 |
| 7. What floor (or room) are we in now? | 1 |
| 8. In which town are we? | 1 |
| 9. In which state are we? | 1 |
| 10. In which country are we? | 1 |
| 11. Repeat the following words: LEMON KEY BALLOON | |
| (The examiner should pronounce the words at a rate of | |
| one per second with up to 5 repeat attempts) | 3 |
| 12. Subtract 7 from 100 and make 5 subtractions | |
| (score 1 for each correct subtraction) | 5 |
| 13. Can you remember the 3 words you have just said? | 3 |
| 14. What is this? (show a pencil) | 1 |
| 15. What is this? (show a watch) | 1 |
| 16. Repeat the following: “NO IFS, ANDS OR BUTS” | 1 |
| 17. Follow a three-stage command: | |
| “TAKE THIS PIECE OF PAPER, FOLD IT IN HALF, AND PUT IT ON THE FLOOR” | 3 |
| 18. Read and obey what is written on this piece of paper | |
| “CLOSE YOUR EYES” | 1 |
| 19. Write a sentence of your choice on this piece of paper | 1 |
| 20. Copy this drawing on this piece of paper (PICTURE) | 1 |
| total score out of 30 | |
Scoring. 0–23 = significant cognitive impairment, high likehood of dementia
source; National Guidelines Committee for acetylcholinesterase inhibitors, January 2000.
original article; Folstein MF Folstein SE McHugh PR Mini-mental state: a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 1975; 12:189–198
Bupropion in smoking withdrawal
DdeC 1 September 2000
-contraindications; epilepsy or factors suggesting increased risk of seizures, use of MAOIs, some psychiatric conditions
-recommened use; started while patient still smoking and stop date set a week later. Should be used in conjunction with psychological support eg weekly.
Treatment should continue for at least 7 weeks. If still smoking then, suggest discontinuation as success unlikely.
-dosage; 150mg (1 tablet) daily for 3 days then BID regularly.
-mechanism; unknown, antidepressant-like action. Perhaps affects dopaminergic reward centre. Perhaps ameliorates noradrenergic withdrawal symptoms of poor concentration and attention.
-interactions. Possible increase in effect (due to hepatic CYP2D6 suppression) of some TCAs, antipsychotics, ß blockers, antiarrhythmics. Other possible interactions.
-side effects; May counteract withdrawal related weight gain. Possible dry mouth, insomnia. Reported tremor, rash/urticaria, headache. Dose-related risk of seizure.
-can be used in conjunction with nicotine replacement eg by patch
-effectiveness; increased rate of not smoking at 1 yr evaluation from 15.6% (placebo) to 30.3% (Jorenby et al. 1999 NEJM 340;685–691)
source: ProCare New Drug Update, July 2000
Cataract, types of
DdeC 22 February 1999
| type | location in lens | symptoms | red reflex | other notes |
|---|---|---|---|---|
| nuclear | nucleus of lens | vision darkened | central dullness | also called ‘sclerotic’ |
| cortical | peripheral cortex | glare, esp. at night | peripheral dark “spokes” | |
| posterior subcapsular | subcapsular | glare, reading difficult | central ‘plaques’ | “PSCC” |
In nuclear cataract, thickening of the lens may cause myopia
source: M McKellar, GP magazine, 1998
Cholesterol; total serum cholesterol by age in NZ (1999)
DdeC 3 October 2004
Chronic fatigue syndrome—differential diagnosis
DdeC 10 December 1997
- autoimmune disease
- endocrine disease
- heart failure
- infection, occult
includes- chronic active hepatitis (eg B or C)
- Lyme disease
- HIV
- TB
- malignancy, occult
- neurological disease
includes- multiple sclerosis
- myesthenia gravis
- Parkinsons
- poisoning
includes- alcoholism
- solvents
- lead or other heavy metals
- radiation
- psychiatric disease
includes- major depressive disorder
- anxiety and panic states
- renal failure
- respiratory disease
includes- obstructive sleep apnoea
- nocturnal asthma
source: Hugh Patterson NZ Doctor (10/12/97)
Colic and reflux in infants and notes on feeding
DdeC 18 February 1998
Colic
Neonatal weight drops up to 10% in first week, should be back at BW by 2/52, then increase at 20–30 g/week.
Need about 6 x 120 ml feeds/day at 4000 g (at 180ml/kg/day).
“Colic” ie prolonged crying (>3 hrs/d, >3 d/week, for >3 weeks—Wessel), usually after 6pm: peaks at 6–8 weeks and resolves by 4 months (‘100 day condition’).
Exclude treatable cause (UTI, starvation), support parents (Weissbluth’s book (Crybabies): your baby is healthy and will thrive, its not your fault, it will pass, you can take steps to cope).
Reflux
Vomiting; if significant there may be a degree of gastro-esophageal reflux.
Exclude infections-AOM, gastro, UTI, meningitis, obstruction-congenital (pyloric stenosis), intermittent (intussusception); less likely are poisoning or metabolic disorder, indicated by failure to thrive.
Hematemesis suggests complication of esophagitis. May be cough or wheeze, apnea, stridor.
— Primary advice: feed upright and burp after feeding: smaller amounts more frequently.
— Secondary measures: ?food thickened with cornflour, gaviscon.
source: pediatrics meeting UofA SOM 17/2/98
Correlation between HbA1c and glucose levels
DdeC 30th May 2004
for 6.5 years measurements were obtained quarterly in 1441 North Americans
| HbA1c, % | glucose, mmol/l |
|---|---|
| 6 | 7.5 |
| 7 | 9.5 |
| 8 | 11.5 |
| 9 | 13.5 |
| 10 | 15.5 |
| 11 | 17.5 |
| 12 | 19.5 |
source Rohlfing CL et al Diabetes Care 25:275 2002 reported in BPAC NZ Evidence that Counts June 2004
Cracked teeth, prevention of
DdeC 24th May 2002
Prevention of cracked teeth
1. If you are a clincher or bruxer (grinder) of your teeth particularly at night time, then have a night guard (bruxing appliance) made to protect your teeth
2. Do not chew on hard objects such as ice, hard candy (jaw breakers etc.) or pop corn kernels
3. Wear protective mouth guards when participating in contact sports to protect your teeth
It should be noted that even with these precautions teeth may develop stress fractures just from everyday use over time.
from http://www.drkimberly.com/cracked.html
Cystic fibrosis mutation testing
DdeC 6 May 1997
12ml EDTA blood to Madhuri Hedge (ph APH x6356) APH molecular genetics (goes to Chch) with details of affected relatives
first result was a heterozygote for Delta F508 mutation, 8/5/00
Deep Vein Thrombosis (‘Economy Class Syndrome’)—DVT/PE associated with prolonged air travel as a passenger
KM/DdeC 15 March 2001
minor risk factors
* age over 40 years
* obesity
* extensive varicose veins
* recent minor surgery
moderate risk factors
* recent heart disease
* pregnancy
* hormone medications and oral contraceptives
* recent leg injury or surgery
* family history of DVT
high risk factors
* previous DVT
* recent stroke
* known clotting tendency
* recent major surgery
* current malignant disease
preventative measures-low risk
* exercise legs periodically during travel
* drink plenty of fluids (not alcohol/caffeine-containing drinks)
* avoid taking sleeping pills while travelling
preventative measures-moderate risk
* use of support or compression stockings
* low-dose asprin
preventative measures-high risk
* heparin administration
* postponement or cancellation of travel
Overall risk is low. See Geroulakis G., The risk of venous thromboembolism from air travel. BMJ 2001 322:188.
source, Anonymous, “Preventing Traveller’s Thrombosis”, in NZ Public Health Report (ed. Mike Baker) 8:p.16 (Feb. 2001)
Dental pain
The unexplained painful tooth
DdeC 24th May 2002
A painful tooth (particularly, sensitive to cold) not explained by decay or infection (i.e. not tender to percussion and dental xrays negative) may be due to
1. exposed dentine due to gum recession, e.g. at the buccal aspect. Examine the alveolar margin
2. a cracked tooth. This may be due to a fracture from trauma or bruxism, or related to fillings in that tooth
Test for this in the following manner; have patient bite down on the tip of a cotton bud held against the four quadrants of the occlusal surface in sequence-cracked tooth will be more painful with occlusive pressure applied to some cusps than to others.
source; Nitin Raniga (Dentist at Lincoln Rd A&E Centre)
Desensitisation treatment for allergic rhinitis
DdeC 13 September 1999
Considered a form of immunotherapy.
Indications
history of rhinitis, hayfever;
treatment of asthma by immunotherapy is NOT recommended
Skin tests
if patient has dermatographism, skin tests not appropriate, RAST tests may be used, requesting individual allergens.
before skin testing, stop antistamines, ßblockers and (oral) steroids for one week.
Technique
desensitisation immunotherapy with allpyral brand kits (contact; Jennifer Hillas, product specialist, Ebos, 415 3267)
contraindications; bronchospasm, use of ßblockers, intercurrent febrile illness, pregnancy, current allergic flare up, bleeding disorders, other immunological disease.
patient to purchase adrenalin injection kit (eg Ana-kit, Ebos, 0800 733–633)
allergens (one or two) for desensitisation are chosen on basis of skin test results (and history)
injections are given with facilities for treatment of anaphylaxis available
induction course is increasing weekly (not less than weekly and not more than three weekly) amounts for 3/12 by subcut. injection deltoid (or lat. thigh)
maintenance course is stable monthly intradermal amounts for 4 years by subcut. injection deltoid (or lat. thigh)
during increase in dosage, if a severe local reaction occurs the next dose is smaller or the same
after injection patient to be observed for 25 minutes before leaving with advice to avoid strenuous activity for 4–6 hours and actions to take in event of reactive symptoms
Log of reactions to be kept and produced at next visit.
Other measures
adjuncts to nasal steroid (rhinocort) and antihistamine (BID loratidine)
also protective sheeting for beds etc from Jackson Allison Co 343 Church St Te Papa phone 622 2277 (‘Jaztec’ brand)
provide brochure “Advice about house dust” (Ebos)t of reactive symptoms.
source: ProCare meeting with Michael Wah and Rohan Ameratunga and literature supplied by Ebos.
Dexamethasone for croup
DdeC 24 February 1997
for mild croup, outpatient treatment, single dose dexamethasone 0.15mg/kg
NB betamethasone equivalent in anti-inflammatory potency (BNF)
source: Geelhoed et al BMJ 313: 140 1996
Diabetes, sugar and the glycemic index
DdeC/PR 29 May 2000
Letter to Brian Edwards, Top of the Morning, via email (totm@radionz.co.nz)
Dear Brian, apropos of your remarks about sugar substitutes being unavailable in cafes and the inconvenience of this for diabetics, you may be surprised to hear that these days we don’t consider table sugar, or sucrose, such a bad thing for diabetics. In fact, some other common foods have a much more marked effect in raising the blood sugar level! This effect, i.e. the effect of different foods on an individual’s blood sugar, can be measured, and is expressed as the ‘Glycemic Index’. Table sugar has a glycemic index of only 65, whereas white bread for example has a GI of 70. Jelly beans have a GI of 80, presumably because they contain a high proportion of the rapidly-absorbed carbohydrate glucose, and the drink Lucozade has a GI of 95.
You can test these observations yourself if you have a portable machine for checking your capillary blood sugar—you will notice some foods give you a large rise in your capillary glucose readings.
More information about the glycemic index is readily available-for example from the book by Jennie Brand Miller [Ref.1 below] or at various websites [Ref.2 below].
Regards, Denis de Castro (doctor) & Pam Russell (Practice Nurse) Three Lamps Medical Centre Ponsonby Auckland
PS We see a different effect of dietary sugar that IS disastrous, namely dental caries in children, and we are now encouraging parents to use only the new sugar-free sweets such as ‘zones’ and ‘zeros’, which we hope will have a widespread effect in preventing this.
- The GI Factor, Hodder & Stoughton 1996
- e.g. Rick Mendosa’s big site at www.mendosa.com
Dietary prevention of recurrence of calcium oxalate renal calculi
DdeC 30 August 2000
Fluid intake increased to 2l/day recommended including fluid intake during the night
Recommended; coffee (plain and decaffeinated), alcoholic drinks such as beer and wine. Lemon juice. (Citrate supplements)
Avoid; apple, grapefruit and orange juice. Soft drinks such as ‘colas’ (high phosphoric acid content). Alkalinising agents such as ‘citravescent’.
Do not take vitamin C supplements.
Moderate protein intake only.
Very reduced salt intake.
Avoidance of calcium now thought not to be helpful.
source: Lyn Lloyd “Careful diet useful in reducing stone risk”; NZ Doctor 30th August 2000 p23
Disease Modifying Anti-Rheumatic Drugs (DMARDs) in rheumatoid arthritis
DdeC 14 June 1999
methotrexate; high efficacy, low toxicity.
sulphasalazine; high efficacy, low toxicity. Adverse effects, nausea (increase dose gradually), skin rash, Stevens-Johnson syndrome, neutropenia (2%) & aplastic anemia.
Monitoring—baseline FBC & LFTs. Repeat FBC every 2–4 weeks for the first three months, then every three months.
hydroxychloroquine; moderate efficacy, low toxicity. Adverse effects, nausea, rash, bone marrow suppression, agranulocytosis, aplastic anemia & corneal and retinal damage at higher doses.
Monitoring—baseline serum creatinine. Routine review by an ophthalmologist every 6–12 months in those taking >6.5 mg/kg/day and /or in the elderly, those with renal impairment, or duration of treatment greater than ten years.
IM gold salts, azathioprine, D-penicillamine; moderate efficacy, high toxicity
source: A Harrison in Medsafe Prescriber Update, No 18, June ’99, pp 4–12
Ectopic pregnancy
Diagnois of ectopic pregnancy with reference to hCG levels and ultrasound
DdeC 22 November 1997
ectopic (usually tubal) pregancy may produce amenorrhea with breast tenderness and nausea
pregnancy test is usually positive
beta-hCG doubles every 48–72 hours in the first few weeks and continues to rise during the first trimester; in ectopic pregnancy this rise may not occur
abdominal ultrasound can show uterine pregnancy at six or seven weeks. Uterine fetal heartbeat can be shown earliest with transvaginal US
extra-uterine signs of ectopic pregnancy are sometimes detectable
- early signs; pelvic pain, vaginal bleeding
- late signs (tubal rupture): syncope, shoulder pain, shock
Emergency Contraceptive Pill (‘Morning-after pill’)
DdeC 1 March 2000
Alternative to Yuzpe regimen is
Levonorgestrel 0.75 mg twice, twelve hours apart.
E.g. Microval or Microlut 25 tablets of 30µg for each dose.
Vomiting only an eighth as often as with Yuzpe and effectiveness is greater (see Lancet 352:428, 8/8/98, Guillebaud comment same issue & abstract in folder)
source: Grimes D, NEJM, Oct. 97 (quoted in MedAlert)
Emollient action by formulation
Activity of emollient preparation types for dry skin
DdeC May 1997
Table; greasiness of formulations (proportional to lipid content)
least lipid, smallest emollient action on skin
— oil in water lotions
— aqueous cream BP
— oily cream BP
— emulsifying ointment BP
— white soft paraffin
most lipid, greatest emollient action on skin
source: ProCare Guidelines 21/11/96
Etidronate (Didronel, Procter & Gamble) for osteoporosis
DdeC 30/1/98
2 tablets daily for 14 days every 3 months.
For the rest of the 3 months, take calcium supplementation (at least 500mg)
Also used in Paget’s, for more prolonged periods.
source: New Ethicals Nov 97
Finasteride, oral, for male-pattern baldness and note on topical minoxidil combination
DdeC 9/3/98
Finasteride (Propecia, MSD).
Indication: alopecia androgenica.
Best effect in partial hair loss.
Differential diagnosis: telogen effluvium after severe illness etc.; drugs such as anticoagulants, chemotherapeutic agents, vitamin A, antidepressants; some medical conditions e.g. diabetes.
Dose. 1 tablet daily (1 mg) for at least 3 months for effect.
Only in males: must not be taken or handled by others esp. pregnant woman as virilistion of fetus may result. Must not have sexual intercourse during pregnancy. Larger dosage is not more efficacious. Effect on hair growth only occurs while treatment continues.
Contraindication: prostatic hypertrophy.
Side effects. Reduced potency or reduced libido.
Mechanism of action: opposes the action of alpha–5-reductase in scalp which converts testosterone to dihydrotestosterone (DHT). Level of DHT in scalp is high in males with alopecia androgenica. DHT shortens growth phase (anagen phase) in hair follicle.
source: Promotional literature, MSD, 9/3/98
Topical combination treatment used by Peter Morgan at Ashley & Marten: 5% minoxidil and 0.025% retinoic acid. Dose 1 ml BID from spray bottle. See Lewenberg, Advances in Therapy Sept/Oct 1996 p 274
Fine needle aspiration (FNA)
DdeC 3 February 1998
Prepare about 6 glass slides, clean and labelled, 5 or 10ml syringe, spray fixative ‘cytofix’ (alcohol not formalin based), alcohol prep swabs and cotton wool.
S McC uses 25g needle for most lesions. May need larger bore needle (24, 23) for more difficult aspirations.
Prepare patient, localize lesion between two digits, check not aneurysmal, alcohol swab to skin, anesthetic not normally necessary (possibly oral benzodiazepine, preferably short-acting, or cutaneous EMLA in child or nervous type).
For medium consistency, vascular lesions (nodes, thryroid, breast fibroadenoma) use needle without syringe attached. Make puncture and multiple (6–10) tracks, trying to locate lesion (eg by feel of a capsule), rotating needle along the track to entrap material. Should take about 30 seconds. Remove needle (Dr Bierre’s pamphlet advocates covering needle hub during removal), attach to syringe containing about 3ml air and gently blow part of specimen onto about the center of a clean slide (should see bloody deposit on slide), then refill syringe with air and repeat onto another slide until no more in needle.
Smear material using the end of another slide; flatten it onto the specimen material a bit then drag a short way up towards frosted end then back down to the other end of the specimen slide. May wish to keep smearer slide for examination also.
Air dry some slides (label ‘AD’) and spray others with alcoholic fixative or place in fixative in a Coplin jar (‘fix’). Air dried preparations are best for lymph nodes-for other tissues fixed slides are also useful. Needle may be washed through with saline to obtain any residual material if necessary.
If special preparation (‘Thinprep’) is available, all aspirated material can be washed into this special collection container instead of being spread onto slides at all.
For soft (lipoma) or hard (fibrous) lesions use needle attached to syringe. Draw back plunger of syringe after entering lesion, probe several times while maintaining tension, and release tension before removing needle from lesion. Then remove syringe from needle to draw up air for making slides as described above.
source: session today at laboratory with Dr Sandy McColl
Folic acid in gastroenteritis
DdeC 30 July 1997
5 mg tds shortened diarrhoea in hospitalised infants in Alice Springs.
Possible mechanism is an effect on intestinal mucosa.
source: News (research report), NZ Doctor 23/7/97 p. 9. Wheaton, G.
Glucosamine for osteoarthritis
DdeC 19 March 2001
Reginster et al. (Liege, Belgium) in The Lancet, Jan. 27 2001 show glucosamine sulphate 1500mg daily for three years improved symptoms and radiology (joint space in knee on weightbearing) in 200 patients compared with placebo in 106 patients with knee OA.
And see review McAlindon, T. The Lancet 357:247–8, 27 Jan 01.
source; NZGP 7 Feb 2001 p. 14
Gonorrhea, current treatment in NZ (2004)
DdeC 10 August 2005
Ciprofloxacin 500mg PO stat and, for likely concomitant chlamydia infection,
azithromycin 1g PO stat.
But where ciprofloxacin resistance is suspected,
ceftriaxone 250mg IM stat plus azithromycin as above.
source: Min Lo, NZ Doctor, 17 November 2004
Hamilton-Norwood rating scale for male-pattern baldness
DdeC 10 March 2004
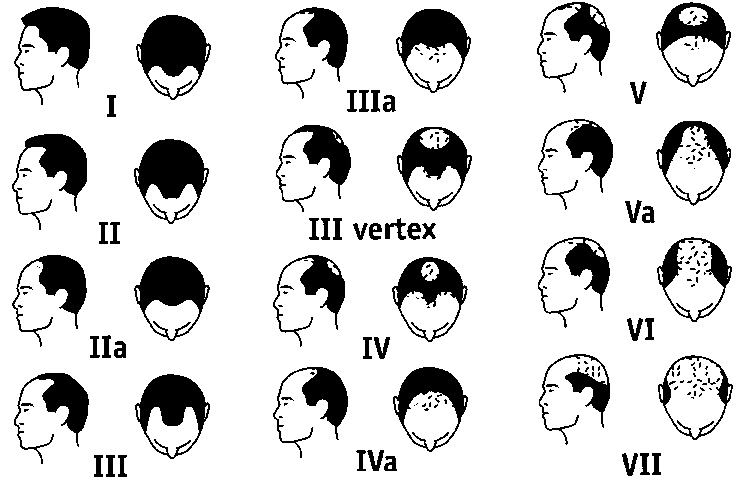
Figure: Diagram showing degrees of male-pattern baldness, rated on Hamilton-Norwood scale.
original article: OT Norwood Male pattern baldness: Classification and incidence. South Med J, 68 (1975)
Helicobacter pylori—triple therapy
DdeC 6 March 1998
omeprazole 20mg BID
amoxycillin 500mg BID
tinidazole 500mg BID
all one week
Hemochromatosis and genetic testing
DdeC 17 Sept 97
Hereditary. Autosomal recessive. Heterozygote is asymptomatic.
Heterozygote rate high in population, approx 10%, so homozygotes (HH) should be 0.25%.
Distinguish from alcoholic cirrhosis with iron overload, where iron saturation is normal, but is raised in hemochromatosis (> approx 0.5, threshold of 0.6 perhaps better if pretest probability low, as in population screen as e.g. acute iron ingestion during deficiency will elevate satn.).
Ferritin higher in HH (but acute phase reactant and high in acute hepatitis).
Increase in iron load is progressive (sigmoidal; symptomatic in 40s in males) and useful to diagnose early as can prevent complications (cirrhosis ± hepatoma, diabetes, impotence, arthralgia—note pattern of 2nd/3rd MCP joints) by venesection, first frequently to remove excess iron load, then less frequent maintenance (for ferritin level <50µg/l or sat <50%).
Mutation responsible for about 85% of HH is Cys282Tyr (C282Y) in HFe gene (was also called HLA-H, as related to HLA genes) established August 1996 [Peter Browett].
Gene mutation test is available. Useful in early phase in males when signs less or in female siblings of cases to predict late onset (clinical disease post-menopausal in female as menstruation delays onset) and for risk to offspring.
Less need for liver biopsy (hepatic iron index-hemosiderin on Prussian Blue stain) which is not greatly accurate. In confirmed case, it has prognostic value—prognosis is worse with cirrhosis. Also worse with DM. After iron excess (eg inappropriate administration) hepatic iron is in RES tissue not parenchyma. Mention of NASH—non alcoholic steatohepatitis (fatty liver).
In HH cirrhosis hepatocellular carcinoma may develop (up to 30%). Consider alpha-feto-protein testing and maybe liver US monitoring 3-monthly. Cys282Tyr mutation is also associated with polycythemia.
source, Meeting on Hemochromatosis, Diagnostic Laboratory, yesterday
Further note, 29 May 2000
Common mutation is C282Y; most cases are homozygous for this but not all homozygotes have clinical features. Homozygotes with H63D mutation do not have features but C282Y/H63D compound heterozygotes represent a small percentage of cases of disease.
C282Y prevalence is highest among North Europeans.
Screening test for hemochromatosis is transferrin saturation (>45, fasting on confirmatory repeat test) with ferritin (?high alcohol intake, other, inflammatory condition). If positive, proceed to C282Y and H63D mutation assays.
source, GM Corbett, Haemochromatosis Update, NZ Family Physician, 27:7–10
Hepatitis C Virus infection, vertical transmission of
DdeC 2 June 1998
Two articles from Diana Rabone:
1. Giacchino R et al, J Paediatrics, 132 (1998):167–9
2. Croxson M et al, NZMJ, ?volume, 9 May 1997: 165–167
Ref 1
Of 70 HCV positive women without HIV or HBV (of 82 suitable subjects found among 7000 women at antenatal wards in Genoa, Italy), all infants were antibody positive at birth, and nine were PCR positive at birth (ie HCV-RNA positive). All these nine children had mothers who were also HCV-RNA positive. Thus 9/45 HCV-RNA positive mothers had HCV-RNA positive infants, but none of 25 HCV-RNA negative mothers.
Of the nine HCV-RNA positive infants, five cleared the disease as assessed by followup PCR testing.
Total congenital infectivity: 4/70 (5.7%)
Ref 2
Studied only HCV-RNA positive mothers.
Two of 30 (6.6%) infants of HCV-RNA positive mothers developed HCV-RNA positivity.
Suggests that HCV-RNA positive mothers do not breast feed because of risk of transmission by this route.
Herpes Simplex Virus serology
DdeC 8 November 2000
Specific serology for HSV1 and HSV2 IgG is available using EIA
HSV1 serological population prevalence about 70%
HSV2 serological population prevalence 10–15%
Interpretation of results
HSV1 -, HSV2 - suggests no hx HSV infection, at least within last 6 weeks (up to 6 months)
HSV1 +, HSV2 - suggests past or present HSV1 infection, probably extragenital (perioral or cutaneous); up to 30% of genital infections are due to HSV1; HSV1 infections of both perioral and genital regions can occur
HSV1 -, HSV2 + suggests past or present HSV2 infection, probably genital infection; occasionally non genital HSV2 infection; or false positive result.
HSV1 +, HSV2 + suggests both (past or present) HSV1 and HSV2 infection; probably perioral HSV1 and genital HSV2; genital infection with HSV1 and HSV2 is possible.
source: N Perkins, NZ Doctor, 27/9/00, p 20
Hip disorders in children, by age of onset
DdeC August 2004
Developmental Dysplasia of the Hip (DDH)
previously known as congenital hip dislocation, CHD)
- age: present at birth (rarely develops later)
- more common in females, with family history of same, and after breech birth
- signs in newborn usually resolve by 9 weeks; about 1 in 1000 babies has continuing signs
- diagnosis by screening tests in infancy and repeated during ‘well-child checks’:
- Barlow and Ortolani tests (before 6 weeks) attempt gentle dislocation and reduction
- Galeazzi’s sign: unequal height of thighs examined in hip flexion
- investigation and treatment: ultrasound scan, radiology; splinting of hips in abduction
Perthe’s Disease: Idiopathic aseptic necrosis of the femoral capital epiphysis
- An osteochondrosis like Osgood-Schlatter’s and Scheuremann’s
- age: 5–10 years, boys>girls, unilateral
- gradual onset of hip pain and reduced range of movement, and gait disturbance
- investigation and treatment:
- xray shows flattening or fragmentation of femoral head;
- conservative (rest, splinting) or operative orthopedic treatment shortens reduces subsequent osteoarthritic changes
Slipped Capital Femoral Epiphysis (SCFE)
- or ‘slipped upper femoral epiphysis’, SUFE
- age: adolescent growth spurt (girls, 11–14 years; boys 13–15)
- onset: subacute (months-weeks) or acute (<3 weeks; ‘unstable’)
- symptoms: pain in hip, groin, thigh or knee; limping
- more common in males, obesity, Polynesians and Africans
- signs: inability to internally rotate hip (rotates externally with passive flexion). Shortened limb.
- investigation and treatment: A-P and lateral radiographs of both hips; surgical pinning of epiphysis
source: Anthony S Children’s Hips Casebook MPS 12:7 (DDH, SCFE) and Merck Manual 17th edition (Perthe’s)
Hypericum perforatum (St John’s wort)—use in depression
DdeC 1 July 1998
Indication, depression
Dosage, 300–1000 mg daily of H. perforatum extract; this contains 0.4–2.7 mg of the active ingredient, hypericins.
Efficacy, about the same as other antidepressant agents-ie about half of patients responded compared with a quarter with placebo.
Side effects, rate was low.
Mechanism, probably action as a SSRI
As with other antidepressants, effect is seen after about two weeks and is maximal at six to eight weeks.
from New Zealand GP magazine, July 1st ’98, p36
refer also Linde, K et al, BMJ 1996: 313: 253–8
Additional Notes
27 November 1998
may cause photosensitivity
18 February 2000
Interactions.
Reduces effect of; oral contraceptives, warfarin, cyclosporin, digoxin and theophylline via cytochrome P450 induction, mainly observed in females.
Interaction with other SSRIs; central serotonin excess (altered mental status, tremor, GI upset, headache, myalgia, restlessness in elderly males).
From MedAlert, 16 Feb ’00 p7.
1 September 2000
Further interactions.
Cytochrome induction may also reduce the availability of antiretrovirals eg indinavir, ritonavir and anticonvulsants eg carbamazepine, phenytoin.
From Medsafe Safety Alert HP 3356 March 2000.
Hypermetropia in young adults—testing with 2 diopter glasses
DdeC 2 May 2001
Instructions to be used with +2D glasses.
Younger patients (less than 30 years old) who achieve a normal distance visual acuity but complain of asthenopic symptoms (headaches/eyestrain/tiredness especially after reading) may have significant hypermetropia.
The patient should be tested binocularly through the +2.00 glasses. A normal result will be the loss of at least five lines of acuity (i.e. the patient can read five lines less because of the blur created by the +2.00D glasses), in contrast if the acuity is better than this it is highly suggestive of hypermetropia. This can be corrected with lenses by an optometrist.
source; Eye Dept., APH, April 2001
Imiquimod. Use for ablation of skin lesions
DdeC 3 March 05
imiquimod 3.75 or 5% is an ‘immune system activator’, acting by several mechanisms.
application: rub in small quantity and leave 6–10 hours (e.g. overnight) and wash off.
solar keratoses: once daily twice a week (e.g. Monday and Thursday) until gone or 16 weeks
basal cell carcinoma, superficial: once daily for five days per week (e.g. Monday to Friday) for six weeks
external genital and perianal warts: once daily three times per week (e.g. Monday, Wednesday and Friday) until gone or for sixteen weeks
not effective in molluscum contagiosum and not thought effective for plantar, plane or common warts.
source: brochure from 3M Co; WP.
Infertility
DdeC/KM/SN 18/7/01
| Clinical Features | |
|---|---|
| Incidence | About 15% of couples present with this at some time |
| Woman’s age | The chance of fertile women conceiving per month falls sharply from around 20% until age 35 to 5% at 40 |
| Time to conceive for fertile women | After six months only 60% of fertile couples will have conceived After 12 months, the figure is 80% After 24 months, the figure is 95% |
| Timing of intercourse | A normal fertility rate is achieved with intercourse every couple of days during the fertile time |
| Duration of infertility | Duration of in infertility is more predictive of the chance of spontaneous pregnancy than the cause of infertility, unless there is “sterility” (eg. blocked tubes, no sperm, etc) |
| Lifestyle | Smoking halves (IVF) pregnancy rates Being overweight affects ovulation and reduces responce to fertility drugs High alcohol or caffeine intake may reduce fertility |
| Cure vs treatment | Few causes of infertility can be cured; but treatment offers a chance of pregnancy similar to that for fertile couples |
| Management | |
|---|---|
| Check | : Female rubella status |
| : Taking Folic Acid | |
| : Weight gain if anovulation | |
| : Occupational and drug history | |
| : Cervical smear history | |
| Advise | : Weight loss if BMI>30 |
| : Stop smoking | |
| : Moderate alcohol and caffeine intake | |
| : Regular intercourse (2–3 times a week) | |
| Investigation | : Length of cycles, Progesterone 6–8 days before menses |
| : FSH and estradiol day 2–4 of cycles | |
| : Semen analysis - repeat in 4–6 weeks unless totally normal | |
| : Prolactin and thyroid function ONLY if irregular cycles | |
| Further Investigation | : Laparoscopy if duration >1yr, unless severe ovulation or sperm factor |
| Refer patient if | : No success after 12 months unprotected intercourse, OR |
| : Any abnormal results on investigation | |
| Early Referral | : Extreme anxiety about fertility |
| : Woman >35 years | |
| : Ovulation factor | |
| : Severe sperm factor | |
| : Previous abdo/pelvic/urogenital surgery | |
| : Previous STD/PID | |
| : Recurrent miscarriage (2 or more consecutive miscarriages) | |
| : Abnormal pelvic/genital examination (woman or man) | |
| : Family history menopause <40 years | |
| : Significant systemic illness | |
| : Genetic conditions (eg cystic fibrosis) | |
| Immediate Referral | : Sperm storage before starting cancer therapy |
Source: Dr R Fisher’s advertisement, July 2001
Itraconazole—oral use in mycoses
DdeC 9 May 2005
in onychomycosis with involvement of toenails: 200mg BID with food for one week, three times at monthly intervals
in onychomycosis, with involvement of fingernails only: 200mg BID with food for one week repeated after three weeks
in vaginal candidiasis: 200mg with food BID for one day or 200mg with food daily for 3 days
in tinea versicolor: 200mg with food daily for 7 days
source: promotional literature from Janssen-Cilag
Jaundice—classification. Hemolytic, hepatocellular and obstructive
DdeC 23/9/1994
| type | bilirubinemia1 | urine colour | stool colour | pruritus |
|---|---|---|---|---|
| hemolytic (excessive production of bilirubin) | unconjugated2 | normal (urobilin)3 | normal5 | no |
| hepatic (hepatitis, cholestasis etc) | both, c > u | dark | variable | possible |
| obstructive (impediment to flow of bile—‘surgical jaundice’) | conjugated | dark (bilirubin)4 | pale (white if total obstruction) | yes |
Notes
1 bilirubin in the blood causes the appearance of jaundice
2 because here the liver’s capacity to conjugate bilirubin is overwhelmed
3 unconjugated bilirubin is not water-soluble. In the gut it is converted to urobilinogen, which undergoes portal recirculation and renal excretion as urobilin.
4 bilirubin is not normally present in urine, but conjugated bilirubin is water soluble and darkens the urine in this case where obstruction leads to absorption into the bloodstream and excretion by the kidneys. However, in obstructive jaundice there is no urobilinogen in the urine, because bilirubin has not been through the bowel and undergone conversion to urobilinogen.
5 most urobilinogen in the colon is excreted after conversion to stercobilinogen and oxidation to stercobilin, which colours the feces.
Clinical summary
— hemolytic jaundice is associated with normal-appearing urine and feces. Tests show unconjugated hyperbilirubinemia.
— hepatocellular jaundice is associated with dark urine and normal or pale fecal colour. High ALT/AST.
— obstructive jaundice is associated with dark urine and light-coloured feces, and pruritus. The blood shows conjugated hyperbilirubinemia and the urine is negative for urobilinogen. High ALP.
Laboratory values for diagnosis of diabetes
DdeC/PR 30th June 1999
values are venous plasma glucose, mmol/l
fasting
≥ 7 diabetes
6.1 - 6.9 impaired fasting glucose
≤ 6 normal
random or 2 hours following 75g OGTT
≥ 11.1 diabetes
7.8 - 11.0 impaired glucose tolerance
< 7.8 normal
source Braatvedt NZMJ 112:171 (28/5/99)
Leptospirosis
DdeC 10 August 2005
An illness of meatworkers, livestock farmers
Occurs after entry of leptospires into abraded skin or intact mucous membranes from urine of infected animals (pigs, cattle, sheep, deer, etc)
May be a subclinical, mild, or severe (icteric) illness. Usually self-limiting
Presentation
Early or mild case; headache, fever, myalgia, conjunctival suffusion
Severe case; meningitis, jaundice, renal insufficiency
Course; 1/52 incubation, 1/52 acute phase followed by ‘immune’ phase with leptospiruria
Diagnosis; serology (‘MAT’) or isolation of organism
Treatment; antibiotics (doxycycline, penicillin) not greatly helpful. May require admission and IV fluids.
source: Accident Compensation Corp., NZ “ACC Review” July 2004
Lithium, living with (by Kay Jamieson)
From the book by Kay Jamison DdeC 7 July 1997
Thanks to Brya Kings who copied out this text by hand
Rules for the Gracious Acceptance of Lithum in Your Life
1. Clear out the medicine cabinet before guests arrive for dinner or new lovers stay the night.
2. Remember to put the lithium back into the cabinet the next day.
3. Don’t be too embarrassed by your lack of coordination or your inability to do well the sports you once did with ease.
4. Learn to laugh about spilling coffee, having the palsied signature of an eighty year old, and being unable to put on cuff links in less than ten minutes.
5. Smile when people joke about how they think they “need to be on lithium”.
6. Nod intelligently, and with conviction, when your physician explains to you the many advantages of lithium in levelling out the chaos in your life.
7. Be patient when waiting for this levelling off. Very patient. Reread the Book of Job. Continue being patient. Contemplate the similarity between the phrase “being patient” and ”being a patient".
8. Try not to let the fact that you can’t read without effort annoy you. Be philosophical. Even if you could read, you probably wouldn’t remember most of it anyway.
9. Accomodate to a certain lack of enthusiasm and bounce that you once had. Try not to think about all the wild nights you once had. Probably best not to have had those nights anyway.
10. Always keep in perspective how much better you are. Everyone else certainly points it out often enough, and, annoyingly enough, its probably true.
11. Be appreciative. Don’t even ‘consider’ stopping your lithium.
12. When your do stop, get manic, get depressed, expect to hear two basic themes from your family friends and healers:
— But you were doing so much better, I just don’t understand it
— I told your this would happen.
13. Restock your medicine cabinet.
Source: Kay Redfield Jamison, An Unquiet Mind; A Memoir of Moods and Madness. Picador 1996
Malaria; treatment of Plasmodium vivax infection
DdeC 2 February 1998
diagnosis; thick and thin blood films in febrile patient arrived out of malarious zone
choroquine regimen: chloroquine phosphate 250mg; iii stat then ii after 6 hours then i BID for two days. Safe in pregnancy
eradicative treatment: primaquine 7.5mg ii daily for two weeks. Not during pregnancy.
source: treatment of patient MS, ex New Hebrides, Jan 92
Medroxyprogesterone acetate (depo-provera IM); management of vaginal bleeding after first dose
DdeC 12 February 97
for heavy bleeding after DP: three-week course of estrogen in moderate dosage to counteract the progestagenic atrophic endometrial effect (eg EED 0.02–0.05 mg daily).
A further course at a lower dosage may be necessary.
If bleeding fails to settle within 10 days the endometrium may be pseudo-decidualised; use progesterone instead of estrogen, eg “Provera” 5 mg daily. If this is successful a further dose of DP may be helpful.
source: J D Hutton, Wellington, 1983 (postgraduate course)
Notes from discussion with Diana Rabone, 6/12/99
try ten days of oral ‘provera’ (medroxyprogesterone) 2.5 mg daily increased if necessary to 5 mg daily, otherwise could use ‘premarin’ (conjugated equine estrogens).
Meningococcal disease, emergency antibiotic treatment
For suspected Neisseria meningitidis septicemia or meningitis
DdeC 21 July 1997
Take sample before treatment for later culture
-throat swab, preferably nasopharyngeal
Emergency treatment for suspected case
- IV or IM benzyl penicillin 1200 mg (2 MU)
- pediatric dose 25–50 mg/kg (0.04–0.08 MU/kg)
- secondary prophylaxis; rifampicin
source: G Durham Dir Pub Health Circular Letter June 1997
Methadone withdrawal as inpatient
Note on inpatient services for withdrawal after methadone stabilisation, known as ‘detoxification’
DdeC 25 May 1998
Usually starts when patient has reached a daily methadone dose of 35 mg
Lasts about ten days
Withdrawal symptoms aided by clonidine and relieved by spa bathing, herbal medicines etc.
Present waiting list for this service about three weeks.
source: from Graham Gulbransen
Nasal fractures and dislocations
DdeC 5 December 2001
xray of nasal bones is not helpful
if the injured nose is frankly distorted (e.g. new devation to one side), arrange for surgical manipulation. This is not done until swelling has resolved (i.e. five days after the injury, after which time there is an interval of about two weeks in which this can be done)
if the injured nose is swollen at the time of presentation and it cannot be determined whether a reduction procedure will be required, review the patient after about four days. Then proceed as in (2) above.
source; Andrew Woollons (at Lincoln Rd A&E Centre)
Nocturnal insulin supplementation of oral agents in NIDDM
DdeC 1 November 1999
One of the great improvements in diabetes management in recent years has been the use of nocturnal insulin, given with either metformin or suphonylureas, in patients who are beginning to fail to respond to oral agents alone. Given that nearly all targets for glycemic control now specify an HbA1c less than 8%, this is an increasingly common situation and, after combinations of sulphonylurea and metformin have been tried, the next usual step is usually the addition of nocturnal insulin.
Giving intermediate insulin (Protophane or Humulin N) at bedtime is associated with a very low risk of hypoglycemia and is usually started at dose of 8 to 16 units, using the fasting glucose the following morning as an indicator of response. The dose should be increased by 2 to 4 units every 5 to 7 days until the target fasting glucose, usually 4.5 to 6 mmol/l, is achieved. This usually requires an average of 30 to 40 units. The dose should not normally be increased beyond 50 units; if a dose greater than this amount is needed, twice-daily insulin is probably needed.
The only problem with this regimen is that the glucose oftern ‘escapes’ in the late afternoon and evening and, if glucose levels are above about 15 mmol/l at this time, twice-daily insulin is usually required. Patients, however, often prefer to start on night-time insulin and will themselves volunteer that there is a need for twice-daily injections. An additional benefit is that they don’t have to carry insulin injection equipment around with them, as the only injection is at bedtime.
Combination therapy with insulin and troglitazone has also proved effective, and combinations with repaglinide and acarbose are also under investigation.
source Drury New Ethicals Journal Oct. ’99. p. 39
Nomenclature
Miscellaneous terms
DdeC 28 June 1999
| common name | term |
|---|---|
| stye | hordeolum |
| chalazion | meibomian cyst |
various sources
Melatonin as a hypnotic and for jet lag
DdeC 5 November 2005
Insomnia
0.3–1 mg nocte
Jet lag
Symptoms; irritability, headache, low mood, fatigue. Increased liability to illnesses
Worse west to east because easier to stay up late than go to bed early!
Take melatonin in the evening in the new time zone
This may hasten readjustment, ie reduce ‘jet lag’
Suggested dosage, 1 mg for each hour that sleep onset is to be moved earlier, in the range 1–6 mg. Halve dose for sublingual preparation.
source: Let’s Live Oct 95 p.34
Addendum 4 August 1999 from Trish Batchelor, NZ Doctor 4/8/99 p29
3–5mg melatonin at bedtime for 4 days after arrival at a new destination.
Addendum 12 May 05, Dee Richards NZ Doctor
2–3mg melatonin at bed time on the first day of arrival and for the next few days
Effectiveness looks convincing, and risks of harm are low
No advantage to beginning treatment prior to travel
No increased effectiveness with larger doses (>5mg) but ‘greater hypnotic effect’.
Ophthamological examination in infants
DdeC 18 February 1998
the general eye exam is helpful: compare size of eyes with each other & with parents’ (should each be 2/3 size of parents eyes)
tests of vision: should follow face. Optokinetic reflex (stripy target) indicates vision & demonstrates eye movements.
Irregular disconjugate eye movements often occur until 3/12 age.
red reflex—useful: through ophthalmoscope at 2 feet from baby, in dim room-light. Use +1 lens, wide beam for both eyes at once.
coloba—a developmental abnormality.
leukocoria—significant; may be from retinoblastoma.
bupthalmos—may be associated with congenital glaucoma.
notes from a lecture by C Hope, February 1998
Opthalmology—common acute problems
DdeC/KM 30 May 2001
Acute allergic conjunctivitis Children/young adults, atopy/other acute allergic symptoms, exposure to allergen, bilateral, onset over minutes, itchy, near normal vision, diffusely hyperemic and watery eye, chemosis (swelling of conjunctivae), lid swelling.
Acute angle closure glaucoma Older hypermetropic (longsighted), usually female, unilateral, onset over one to two days, severe visceral eye pain and nausea, headache, haloes, decreased vision, deeply and evenly injected eye, cloudy cornea, firm eye, oval/dilated pupil.
Corneal foreign body Any age, history of grinding/sanding/dusty environment, normally instantaneous onset, usually unilateral, pain on blinking, near normal vision, focally hyperemic (adjacent to foreign body), watery eye, ± fluoroscein staining.
Corneal ulcers Any age, history of HSV/trauma/contact lens wear, unilateral, onset over one to two days, foreign body sensation, pain, photophobia, decreased vision, mild to moderate diffuse injection, cloudy cornea, fluoroscein staining, pain relief with topical anesthetic, hypopyon.
Episcleritis Adults, unilateral, onset over one to two days, dull ache, normal vision, sector of redness.
Giant cell arteritis Elderly patient, symptoms of polymyalgia rheumatica, scalp tenderness, headache, jaw claudication, sudden onset, usually unilateral, marked visual loss, afferent pupillary defect, field loss, swollen optic disc, raised ESR/CRP.
Hemorrhagic/exudative (‘wet’) age-related macular degeneration Elderly patients, ± history of ‘dry’ macular degeneration, sudden onset, unilateral, dense central visual loss, white eye, sub-macular blood, ± atrophic or old exudative maculopathy in fellow eye.
Herpes zoster ophthalmicus Elderly patients, onset over one or two days, unilateral, facial/periocular pain, normally mild visual loss, vesicles in distribution of ophthalmic nerve, puffy lids, mucopurulent discharge, conjunctivitis, occasionally signs of iritis (see below).
Infectious conjunctivitis Any age, onset over one to two days, normally bilateral (but one eye first), foreign body/gritty sensation, sticky lids and watery/mucopurulent discharge, mild photophobia, near normal vision, redness maximal in fornix, normal pupil, URTI/preauricular lymph nodes, discomfort relieved with topical anesthetic.
Iritis Adults, history of iritis, onset over one to two days, usually unilateral, photophobia, watery eye, dull pain, mild to moderately decreased vision, ciliary (circumcorneal) redness, small pupil, posterior synechiae.
Ophthalmic artery occlusion Older/atherosclerotic patients, sudden onset, unilateral, moderate-severe vision loss, white eye, afferent pupillary defect, attenuation of retinal arteries, retinal pallor (signs often minimal).
Ophthalmic vein occlusion Older/atherosclerotic patients, sudden onset, unilateral, mild-severe vision loss, white eye, possible afferent pupillary defect, dilated and tortuous retinal veins, retinal haemorrhages, cotton wool spots.
Optic neuritis Young adults, symptoms of demyelination elsewhere, unilateral, onset over one to two days, disturbance of colour vision, pain on eye movements, mild to profound visual loss, white eye, colour desaturation, afferent pupillary defect, disk usually normal.
Papilloedema Adults, headaches, bilateral, onset over days to weeks, transient loss of vision on standing, normal vision and pupils, enlarged blind spots, swollen optic discs, ± sixth nerve palsy.
Penetrating eye injuries Any age, use of high-speed tools/hammering, usually unilateral, immediate but patients often present several days later, transient pain, floaters/flashes, mild-severe visual loss, eye may be white/hyperaemic/deeply injected or bloody, peaked pupil (see below), cataract, loss of red reflex, vitreous haemorrhage, intraocular foreign body.
Posterior vitreous detachment Fifth to sixth decade, myopia, recent trauma, unilateral, flashes/smaller (often ring or arc shaped) semi-transparent floaters, painless, white eye, normal vision/visual fields/ophthalmoscopy.
Retinal detachment Adults, high myopia, recent trauma, unilateral, onset over one to seven days, flashes/floaters/field loss/failing vision, white eye, abnormal red reflex, holes in or detachment of retina.
Solar keratitis (Arc eye/snow blindness) Young adults, recent skiing/mountaineering/welding/suntanning, bilateral, onset four to eight hours after exposure, progressive onset, pain, photophobia, copious tearing, aversion to opening eyes, symptoms largely resolved by instillation of amethocaine, near normal vision, hyperaemia, diffuse fluorescein staining in palpebral aperture.
Vitreous haemorrhage Fourth to sixth decade, diabetics, myopia, recent trauma, unilateral, flashes/larger and more dense floaters, painless, white eye, mild to severe vision loss, near normal visual fields, large floaters in or loss of red reflex.
source; Malcolm McKellar, NZ GP, 30 May 2001, p 29.
Addendum
Peaked pupil A “peaked pupil” is an oval or pear-shaped pupil which is associated with prolapse or incarceration of the peripheral iris in the penetrating wound. The usual mechanisms include rapid loss of aqueous carrying the peripheral iris into the wound, a foreign body dragging the peripheral iris into the wound and occasionally in severe trauma vitreous loss prolapsing the iris. The peak of the distorted pupil points directly at the penetrating wound. Peaked pupils are also seen in some patients following intraocular surgery.
(personal communication, M McKellar 11/6/01)
Orlistat (Xenical, Roche) a new drug for obesity
DdeC 13 March 1998
physiology: lipase inhibitor, ie nonsystemic action
prevents about 30% of fat absorption
dosage; 120 mg (1 tab) tds with or after meals
- could be used less often to save money (eg with main meal only)
side effects: steatorrhea, “oily spotting”. Expected to be transient as user adjusts fat intake…
Fat-soluble vitamin malabsorption not a problem.
Orthopedic guidelines
Notes on acute orthopedics for use in the Accident and Emergency Clinic.
DdeC 5 December 2001. Revised, 21 June 2002
Contents
List of abbreviations
General notes
Shoulder: fracture of clavicle, dislocation of acromioclavicular joint, dislocation of shoulder
Upper arm: fracture of neck of humerus, fracture of shaft of humerus, supracondylar fracture
Radius and ulna: fracture of head of radius, mid-shaft fracture, Monteggia fracture, Galeazzi fracture
Wrist and hand: Colles fracture, Smiths fracture, fracture of scaphoid, Bennetts fracture, fractures of metacarpals, fractures of phalanges
Pelvis: major pelvic fractures, minor pelvic fractures
Lower Limb: fracture of neck of femur, dislocation of hip joint, fracture of shaft of femur, supracondylar fracture, fracture of condyles, fracture of patella
Abbreviations
AC, acromioclavicular
MUA, manipulation under anesthetic
ORIF, operative reduction and internal fixation
POP, plaster of paris (cast)
General notes
Recommended times etc are for adult patients
Immobilisation time is usually shorter for children
- Shoulder
fracture of clavicle
broad-arm sling 3/52
review at fracture clinic in 5–6/7
get orthopedic advice if
-skin tethering over fracture
-fracture in distal third
-large hematoma
-neurological abnormalities in arms, or
-very wide separation
dislocation of AC joint
broad-arm sling 2–3/52
if widely dislocated, review at fracture clinic.
very few need surgery.
dislocation of shoulder
may reduce spontaneously lying prone with affected arm weighted over side of couch
otherwise pre and post reduction films. Sedation and muscle relaxant, e.g. midazolam, diazepam, antiemetic IV
first dislocation; shoulder sling and body bandage to prevent external rotation. Sling for 3–4/52 with fracture clinic check at 10/7
recurrent dislocations; broad-arm sling and fracture clinic appointment.
-Upper arm
fracture of neck of humerus
collar & cuff sling 2/52; mobilise early (esp. older people)
review 10/7 and xray to ensure humeral head has not displaced
fracture of shaft of humerus
check for neural/circulatory deficits
U-slab plaster and collar and cuff sling for 2–3/52 then functional brace for 6–8/52
supracondylar fracture
- if undisplaced
short collar and cuff sling possibly with above elbow backslab at >90° flexion 3–4/52
with review and xray through POP at 1/52
- if displaced
check for neural/circulatory deficits
splint for comfort and arrange orthopedic admission
fracture of olecranon
orthopedic admission for ORIF
dislocation of elbow
careful check for vascular compromise
reduction under sedation, plaster backslab at 90°
or
orthopedic admission, splint for comfort in ambulance
-Radius and ulna
fracture of head of radius
- if comminuted or displaced, orthopedic admission
- otherwise
collar and cuff 2/52 and pronation/supination exercises
mid-shaft fracture
if one bone and undisplaced, above elbow padded POP 1/52 and review with xray through POP, 6/52 total in cast
otherwise orthopedic admission for ORIF (adult) or MUA (child)
Monteggia fracture (fracture of ulna associated with dislocation of radial head)
orthopedic admission
Galeazzi fracture (fracture of radius associated with subluxation of inferior radio-ulnar joint)
orthopedic admission
-Wrist and hand
Colles fracture (fracture distal end of radius with dorsal angulation)
if undisplaced, dorsal slab moulded into palmar flexion and ulnar deviation
if reducible, closed reduction and well padded POP moulded into palmar flexion and ulnar deviation. Xray for position post reduction and at 10/7. Total 5–6/52 in cast
otherwise (comminuted, marked displacement) orthopedic admission for ORIF or external fixation.
Smiths fracture (fracture distal end of radius with ventral angulation)
if undisplaced, ventral slab
if reducible, closed reduction and POP in extension. Below elbow POP unless fracture >2.5 cm from wrist then above elbow POP. Xray for position post reduction and at 10/7. Total 6/52 in cast
otherwise (comminuted, marked displacement) orthopedic admission for ORIF or external fixation.
fracture of scaphoid
about 95% are apparent on initial xray (scaphoid views)
if displaced, orthopedic referral for ORIF with Herbert screw
if undisplaced, scaphoid plaster for 6–8/52. If un-united then refer to orthopedic surgeon
if no fracture on xray but clinical suspicion (tenderness in anatomical snuffbox), scaphoid plaster 2/52 and re-xray out of plaster
in children, scaphoid fractures very uncommon with open growth plates. Do not plaster on suspicion-crepe and repeat xray in 10–14 days
Bennetts fracture (intra-articular fracture/dislocation of base of first metacarpal)
if displaced, refer for ORIF
otherwise reduce deformity if possible and apply extended Bennetts POP with orthopedic felt over reduction points Post reduction film through POP and admit if reduction not satisfactory. Period of immobilisation 5–6/52
fractures of metacarpals
check xray for dislocation of CMC, especially 5th
base or neck of metacarpals; crepe bandage and high-arm sling for 3–4/52
shaft of metacarpals; if transverse, midshaft and angulated requires ORIF with plating. Otherwise, if spiral, crepe and high-arm sling. Watch for rotational deformity. Review at fracture clinic within 3–4/7
head of metacarpals; if displaced, refer for orthopedic opinion. Otherwise, crepe and elevate for 4–5/7 then mobilise. If head of 5th metacarpal is ventrally angulated >40° (‘punch fracture’), it can be reduced under plain lidocaine local anesthesia and thick ulnar POP slab applied and moulded to maintain position of the reduced fragment.
fractures of phalanges
obtain orthopedic opinion, especially if involving a joint. Will require 3/52 immobilisation
-Pelvis
major pelvic fractures
BP observations. IV line for possible fluid replacement. Oxygen. Analgesia. Nil by mouth
hospital admission by ambulance
minor pelvic fractures (isolated fracture of pubic ramus, avulsion fractures)
analgesia, bedrest, district nurse
may need admission
-Lower limb
fracture of neck of femur
analgesia, IV fluids, oxygen, nil by mouth
splint and admit by ambulance
dislocation of hip joint
orthopedic emergency
check for neurological deficit
analgesia, IV fluids, oxygen, nil by mouth
admit by ambulance
fracture of shaft of femur
BP observations, analgesia, 2–3 l fluid IV, oxygen, nil by mouth
document neurovascular status especially before femoral nerve block
splint with Hare traction and admit by ambulance for ORIF and immobilisation ≥12/52
supracondylar fracture
admit for traction or ORIF
distal fragment often rotated due to pull of gastrocnemius
in children may be undisplaced and treated with Bohler cast.
fracture of condyles
analgesia, document neurovascular status, NBM
splint & admit for possible ORIF (may be treated conservatively if undisplaced and unicondylar)
fracture of patella
undisplaced: contoured Zimmer splint for 6/52
may need aspiration if tense hemarthrosis
if displaced or comminuted, refer for ORIF
dislocation of patella
if first time, consider referral for repair
reduction
skyline xray for intra-articular osteochondral fragments; may require arthroscopy
splint or Bohler POP (well moulded about lateral border of patella and change if loose) for 6/52
fracture of tibial plateau
splint and admit for orthopedic treatment
often associated with medial or cruciate ligament rupture and fracture of fibular neck
will require 6–8/52 immobilisation
fracture of tibial shaft
consider admission for all tibial fractures
if displaced, comminuted, angulated or very swollen admit-NBM, IV fluids, oxygen in ambulance
otherwise
in children, above knee padded POP 1/52 then above knee walking plaster 4–8/52 depending on age
in adults, above knee padded POP 2–3/52 then total contact (Sarmiento) walking POP 3–4/52
undisplaced fractures require regular check xrays for maintenance of position
fracture of lateral malleolus
careful evaluation-may require ORIF
below knee padded POP 2/52 well moulded about lateral malleolus, then walking POP 3–4/52
fracture of medial malleolus
if any displacement requires ORIF
below knee padded POP 1–2/52 (may take longer for swelling to reduce) then walking POP 3–4/52
fracture dislocation at ankle
if the toes are without circulation the dislocation must be immediately reduced
fracture of calcaneum
most os calcis fractures require admission to treat injuries elsewhere
if bilateral admit for bedrest
if comminuted or displaced admit for ORIF
if undisplaced, crepe, crutches and bedrest
fracture of metatarsals
transverse fracture of midshaft of 5th metatarsal (Jones fracture) may require ORIF
widely displaced fracture of base of 5th metatarsal may require ORIF
fracture of first metatarsal or displaced fracture of fifth metatarsal-below knee padded POP followed by walking POP
otherwise crepe bandage and crutches 4–6/52 for comfort
crush injuries of foot (run-over)
may need admission because of swelling
examine lateral xray carefully for tarso-metatarsal (Lisfranc) dislocation
source; guidelines of Lincoln Rd White Cross A & E Centre (previously WestCare), Auckland
Pitted keratolysis
DdeC/BF 26 July 2000
Caused by Micrococcus sedentarius and affects the toewebs and the plantar skin of the ball and heel of the foot
Hyperhidrosis is a predisposing factor and therefore it is frequently seen in those who almost exclusively wear occlusive trainers or who spend their working day in footwear such as gumboots
Patients often complain of strong foot odour associated with a burning sensation and tenderness of the soles
Clinically the skin is white and macerated and studded with pits giving it a “moth-eaten” appearance
The diagnosis is usually a clinical one although tinea and erythrasma (Corynebacterium minutissimum) will need to be excluded if the toewebs are involved
Treatment consists of twice daily application of benzoyl peroxide, erythromycin or fusidic acid for a minimum of a week
If the condition is particularly florid, the author finds potassium permanganate soaks (1/10,000 aqueous solution) twice daily before the topical application very effective
Prevention of further attacks can be obtained with advice on footwear, and the use of aluminium chlorhexahydrate solution to reduce sweating
Washing the feet with a benzyl peroxide soap bar may also be helpful.
source; NZ Doctor19 July 2000 p 18
Polycystic kidney disease
DdeC June 2000
genetics; two types—autosomal dominant (common, any age) and autosomal recessive (less, common, may be detected at birth)
diagnosis; family history, ultrasound
sequelae; hypertension, calculi (may be radiolucent urate), hematuria after trauma, infection, end stage renal failure
autosomal dominant form inherited in half of offspring but variable penetrance
associations; diverticulosis, hepatic & pancreatic cysts, intracranial arterial aneurysms with subarachnoid hemorrhage
management; maintain fluid intake and control HBP eg ACEI, genetic counselling
source: Wallace NZ Family Physician 27:10
Polycystic ovary syndrome
DdeC March 2001
symptomatology; oligomenorhea (less commonly, amenorrhea), hirsutism, acne (androgenic effects)
pathology; ovary contains peripheral follicles and increased stroma
examination; obesity (BMI>30), hirsutes
investigations;
- raised LH and testosterone in 50% of cases
- polycystic ovaries on USS (note; normal endometrial thickness is <12mm)
- day–21 progestagen can be used to confirm anovulation
management;
- regular withdrawal bleeds can be induced by combined OC or luteal phase progestagen (eg ‘provera’ 5 mg od for 5/7)
- ovulation can be induced with clomiphene; works better when BMI<32. Clomiphene is given as 25–50mg on cycle days 2–6. If unsuccessful, gonadotrophin or laparoscopic ovarian drilling
- experimental treatment; metformin for wt reduction and induction of ovulation
- for hirsutism; antiandrogens effective including cyproterone containing OC. Acne responds more quickly (6/52) than hirsutism (12/12)
source: Cindy Farquhar, Auckland; Menstrual Disorders. NZ Doctor 28/3/01 p. 20
Pot sizes
Sizes of pots for dispensing creams etc
DdeC 7 May 1997
small pot, 25 g
medium pot, 100–200 g
large pot, 500 g
Prophylaxis of bacterial endocarditis with antibiotics before dental and certain other procedures
DdeC 9 August 1999
standard; oral amoxycillin 2g one hour before procedure and 1g six hours later
suspected or mild penicillin sensitivity; oral cefuroxime axetil 1g one hour before procedure and 1g six hours later
previous anaphylactic reaction to penicillin; oral clindamycin 300mg one hour before procedure and 150mg six hours later or oral clarithromycin 500mg one hour before procedure as a single dose
note, more intensive regimens (eg oral or IV amoxycillin 2g and IM or IV gentamicin 2mg/kg up to 120mg within 30 min of procedure) are recommened for high risk patients with previous endocarditis or prosthetic valves etc.
source; National Heart Foundation of NZ, August 1999
Pruritis, symptomatic treatment
DdeC 23 January 1998
cream
hydrocortisone 2%
menthol 1%
phenol 0.5%
in aqueous crm
tablets
doxepin 25–50mg nocte
source: John Snow letter on patient BF, 20/1/98
Renal function and nephrotoxic agents
DdeC/KM 23 Apri 2001, 23 May 2001
Plasma creatinine
Plasma creatinine reflects its production (proportional to the muscle mass containing its precursor, creatine, as opposed to creatinine) and excretion [proportional to glomerular filtration rate (GFR)]. Those with large muscle mass will have greater plasma creatinine levels. With age, the proportion of muscle mass in the body decreases, so a lower plasma creatinine is expected. If renal function falls, the GFR falls, so plasma creatinine increases.
Glomerular Filtration Rate
The glomerular filtration rate is the flow rate of filtered fluid through the kidney. It is measured as ml/min and can be corrected for body mass as ml/min/1.73 m2body surface area. It falls with reduced renal function.
It can be approximated by the creatinine clearance rate, the volume of plasma that is cleared of creatinine per unit time: ie the rate of clearance of creatinine by the kidney.
GFR decreses with reduced renal function
Expected GFR (Merck Manual 17th edn.):
- Males 82–125 ml/min
- Females 75–115 ml/min.
Expected GFR for age GFR = (157 - 1.16 x age [years]) ml/min per 1.73m2
Modified Cockcroft-Gault formula for estimation of GFR given age, weight, sex and plasma creatinine
GFR (ml/min) = (140 - age [years]) x weight (kg) (x 1.25 in males) / plasma creatinine (mmol/l) x 1000
Generally it is advised to review medication when GFR < 60 ml/min and to consider reducing or stopping some medication when GFR is < 30 ml/min.
Proteinuria
Estimation of 24 hour urine protein from casual sample (Pidgeon), based on the ratio of protein to creatinine
protein excretion (g/day/1.73m2 surface area) = [urine protein (mg/l)/urine creatinine (mmol/l)] x 0.0088
More than 150mg daily generally indicates glomerular disease; nephrotic range is greater than 3g/day
In diabetics, 30 to 300 mg daily is considered microalbuminuria
Greater than this indicates diabetic nephropathy.
Nine Important Nephropathic Agents
Nephrotoxic
- Radiocontrast agents - use low ionic agents, avoid dehydration
- Non-steroidal anti-inflammatory drugs - use paracetamol
- ACE inhibitors - check renal function
Need adjustment if GFR is reduced
- Allopurinol - 100mg/day per 30ml/min of GFR
- Digoxin - check levels
- Sulphonamides - halve dosage if GFR is < 30ml/min
Not used if GFR < 30ml/min
- Some hypoglycaemic agents - chlorpropamide, glibenclamide, metformin
- Potassium-sparing diuretics - amiloride, triamterene, spironolactone
- Tetracyclines
source: Pat Phillips (Woodville NSW) in New Ethicals Journal, April ’01, p. 40.
and Grant Pidgeon (Wellington) in New Ethicals Journal, June ’01, p. 47
Salisbury approximation for pediatric dosage
DdeC 22 August 1997
Dose is percentage of adult dose, calculated thus:
under 30 kg body weight, use (body weight x 2)% of adult dose
over 30 kg body weight, use (body weight + 30 kg)% of adult dose
source: GP Weekly, 20/8/9/7 p 14
original article: J. A. Lack & M. E. Stuart-Taylor, Calculation of drug dosage and body surface area of children, British Journal of Anaesthesia 1997; 78: 601–605
Skin, care of dry
DdeC June 1996
One of the most common causes of dry skin is overwashing. Using strong soaps and washing with very hot water both reduce moisture in the skin. Addressing this problem can be simple. Cooler bathes or showers coupled with the use of mild unperfumed soaps such as Dove or Neutrogena only under the arms, groin and around the anus. Other parts of the body don’t need to be washed with soap unless dirty or after exercise. After bath or shower apply a waterbased moisturising lotion (Sorbelene, Neutrogena, etc.) to the entire body. Then using a damp towel, wipe off any excess lotion that hasn’t penetrated the skin. Using a damp towel prevents evaporation of the lotion from the skin which would in turn result in dryness,
source: Colin Batrouney, HIV Herald 6 (Feb. 1996)
Serotonin syndrome, the
Features of the ‘Serotonin Syndrome’ (serotoninergic toxicity)
Drugs that may be causitive
Treatment
by DdeC/ED 27 June 2000 - 18 June 2001 - 30 May 2004
Description
Occurs with excessive brain serotonin levels following interaction of agents that facilitate serotonergic neurotransmission.
Often occurs within a day of change in treatment (initiation or increase of dose of one agent or addition of another serotonergic agent).
Compare neuroleptic malignant syndrome: an idiopathic response to a neuroleptic agent, usually develops over days or weeks after longer periods of treatment.
No laboratory test is diagnostic at present.
Features that may be present in the syndrome
neurological;
• mental state changes-agitation, anxiety
• incoordination, myoclonus, hyperreflexia, ocular clonus
• tremor (fine; around 12 hz)
autonomic;
• diaphoresis
• shivering
• fever, usually low-grade (central effect plus hypermetabolism of muscle)
cardiological;
• tachycardia
gastrointestinal;
• diarrhea
respiratory
• (in severe cases) hypercapnia (increased muscle activity plus respiratory muscle hypertonia)
Drugs that may be involved in causing the syndrome
• antidepressants:
- SSRIs (fluoxetine etc)
- MAOIs (including moclobemide)
- TCAs (esp clomipramine, imipramine, amitriptyline)
- SSNRI (venlafaxine)
- St John’s wort
• antiparkinsonian agents:
- selegeline
- bromocriptine
- levodopa
- amantadine
- carbergoline
- pergolide
• recreational drugs
- cocaine
- hallucinogenic amphetamines such as MDMA (ecstasy)
- LSD
• migraine treatments
- dihydroergotamine
- sumatriptan
- zolmitriptan
- naratriptan
• analgesics
- tramadol
- pethidine
- pentazocine
- fentanyl
• appetite suppressants
• others
- carbamazepine
- lithium
- sibutramine
- buproprion
- buspirone
- dextromethorphan
- l-tryptophan
Treatment
- stop the inducing agents
mild (eg overdose of single SSRI)
- reassurance
moderate (agitation, hypertonia, clonus, tachycardia)
- oral cyproheptadine, 8–16mg, or benzodiazepine
severe (with increasing hyperthermia)
- IV chlorpromazine 25–50mg up to 100mg in ICU. Muscle paralysis.
sources
(1) New Ethicals Journal, June 2000. p. 59.
(2) “Toxicology Quiz”, Geoff Isbister. NEJ June 2001 pp 65, 87
(3) Aust Adv Reac Bull 23 Feb 2004 reported in BPAC NZ Evidence that Counts 4: June 2004.
Smoking cessation
DdeC 17 December 1997
Triage
divide smokers into 3 groups
• not ready
• unsure
• ready
with the question
How do you feel about your smoking?
Withdrawal symptoms
are worst in the first 2 or 3 days
last about 2 weeks
except craving, which can last years
Indicators of severe dependency
use of >20 cigarettes daily
previous craving after stopping
first cigarette smoked <25 min after waking
Motivational interviewing
ask for pros and cons, summarize, and ask
‘where does that leave you?’
Recommed smoker return on Quit Day with patch
Nicotine replacement
‘Nicabate’ patch. Costs about $37/week
1–11/2 daily for eight weeks
Remove at night if nightmares occur
Notes from Stop Smoking Program by Colin Mendelssohn UNSW, meeting on 22/10/97
Snoring, treatment by radio frequency tissue volume reduction
DdeC 27th September 2004
Procedure ablates two strips of the patient’s soft palate with radiofrequency burns under local anesthesia. Cost (2004) $600
source: NZ Doctor 14 July 04 p.4. Drs Neil Hutchinson and Andrew Murley, Waiake Medical Centre, Torbay, Auckland
Temperature, tympanic, normal range
DdeC/CQ 11/2/98
| age, years | normal range |
|---|---|
| 0–2 | 36.4°C- 38.0°C |
| 3–10 | 36.1°C- 37.8°C |
| 11- 65 | 35.9°C - 37.6°C |
| >65 | 35.8°C - 37.5°C |
source: Braun thermoscan product guide
Thromboembolic causes of retinal blindness
DdeC 28 June 1999
- central retinal artery occlusion
onset; sudden
clinical background; atherosclerosis, uncommonly temporal arteritis
appearance; constricted arteries in milky white edema with cherry red macular spot - central retinal vein occlusion
onset; less sudden
clinical background; HBP, DM, atherosclerosis in elderly
appearance; retina hemorrhagic, tortuous veins, may be edema
note; may be rubeosis iridis and secondary glaucoma
source: Lim & Constable; Colour Atlas of Ophthalmology
Troponin, diagnostic levels in myocardial infarction
DdeC September 2000
What is cardiac troponin?
An element of fine muscle architecture. It binds with actin in the shifting filament mechanism. Cardiac troponins T and I differ from skeletal T and I (but C in common).
Use as diagnostic indicator of cardiac muscle damage
• sensitive; more sensitive than CK or CKMB. Two negative results within 12 hrs exclude MI
• specific; only arises from cardiac damage (cf CK, affected by skeletal muscle damage). Not normally present in blood. May be found in stable angina, indicating some damage and risk of subsequent MI. Rarely may be false positive in renal failure and some inflammatory muscle diseases. Also in CHF, cardiomyopathy, post resuscitation; elevation may indicate cardiac damage
• rise time is like CK/CKMB ie takes 4–12 hours after onset of infarct to become positive
• continues positive for a week or so post MI (cf CKMB negative again after about 2 days)
source: Dr C Kyle; Diagnostic Medlab Medical Bulletin August 2000
Vitamin D3 levels
DdeC/ED 30 November 1998
Low levels are associated with rickets and osteomalacia
Check vitamin D3 levels (serum 25-hydroxy D3) in elderly ‘shut-in’ patients
If low use plain vitamin D (calciferol), 10µg daily or one 1.25 mg tablet monthly
In established osteomalacia ALP is increased and phosphate decreased.
Warfarin—dietary stabilising factors
DdeC 23 June 1999
Foodstuffs rich in vitamin K, e.g. broccoli, spinach, brussels sprouts and lettuce, are thought to help to stabilise the efffect of warfarin as an anticoagulant.
source; P Ockelford, Diagnostic Laboratory Mini-News, June ’99
Warts, topical applications
Gentle wart paint
DdeC/PR 27 February 1998
salacylic acid 1 part
lactic acid 4 parts
in flexible collodion
pare wart surface gently and apply a small amount with a matchstick
source, S Helander. 12/02/98
Paste for plantar warts
DdeC 27 July 1998
70% salicylic acid
liquid parraffin ad 100%
apply weekly under occlusive plaster
no further dressing needed
pare before reapplication.
source, J Wishart, letter of Nov ’88
Xerostomia. Use of pilocarpine solution and other measures
DdeC 19 September 2002
Pilocarpine:
dose required is variable among individuals, 2.5mg/dose to 10mg/dose PRN QID & N
in excess causes sweating, nausea, diarrhea, may be u. urgency and vivid dreams, exacerbation of bronchospasm
Other measures for xerostomia:
sugar free chewing gum or sweets
water, sparkling mineral water, low fat milk
Other pharmaceutical approaches:
new cholinergic – Cevimeline
chewing gum with casein derivative releasing calcium and phosphate – Recaldent
calcium phosphprotein paste – Topacal-C5
source: Ferguson M, NZFamPrac 29:258 (August 2002)